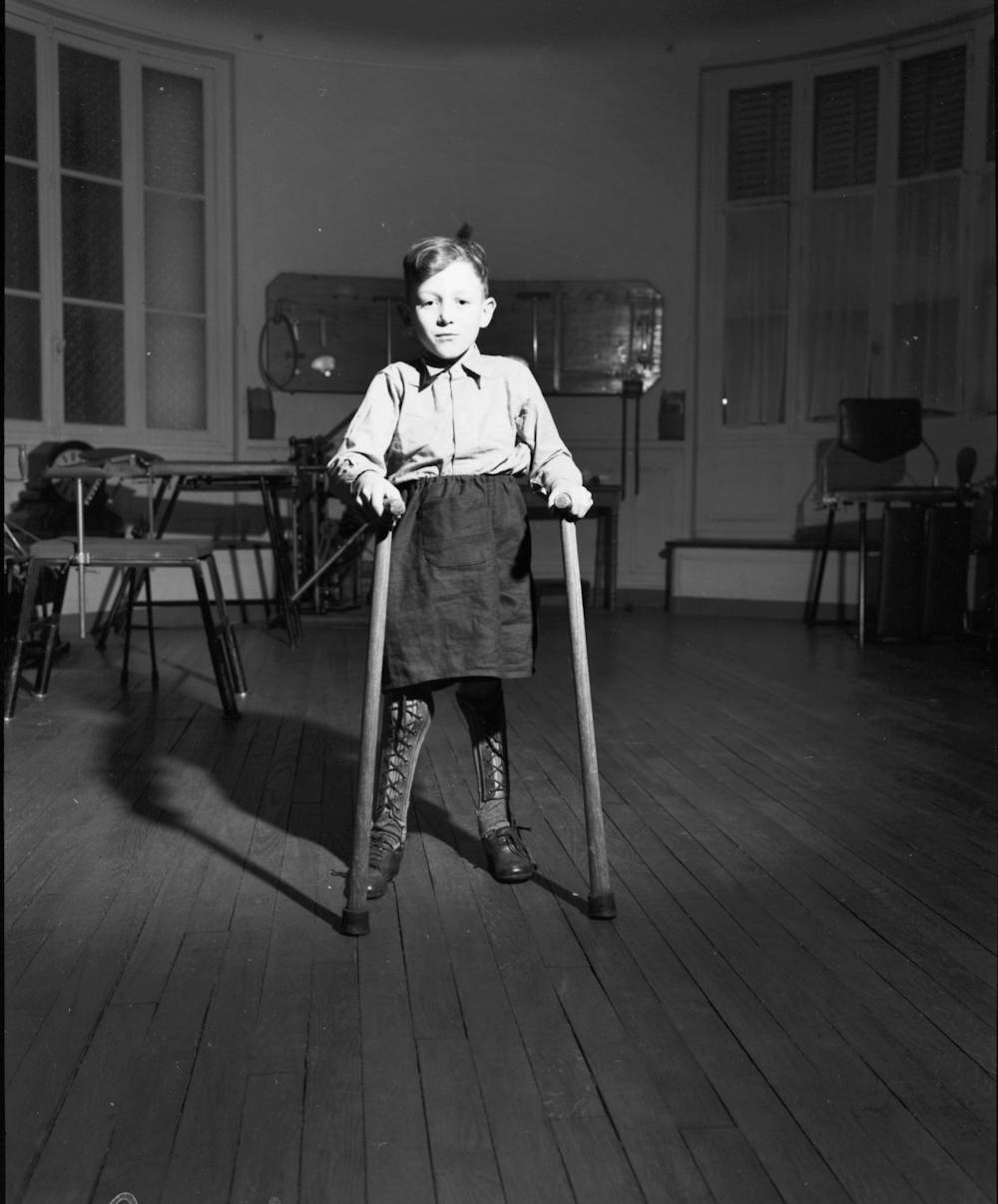
June 1944 brought a quickly escalating polio outbreak to Catawba County in North Carolina. Three doctors conceived of a plan to form an emergency hospital in Hickory.
Although most hospital administrators preferred not to take polio cases, this one would cater specifically to them. Setting it up meant emptying out a summer camp that was built as part of President Franklin D. Roosevelt’s Works Progress Administration.
As legend has it, Dr. H.C. Whims, a health official involved in setting up the hospital, called the woman who was running the camp and asked her to clear it out. She said the campers were picking blackberries and she’d promised them a cobbler — but once they got their cobbler, she’d send them home.
And when she did, the patients started pouring in.
What stands out about the hospital is how quickly it developed — the first patients were admitted to Hickory less than three days after the doctors decided to open a hospital. By 1945, it had treated hundreds of patients and Hickory proudly wore the title of “Polio City.”
Life magazine featured the town’s response, and writers would continue to chronicle the “Miracle of Hickory,” given its name in a March of Dimes pamphlet, for decades to come.
Moury was one of the first patients of the nationally known medical marvel. When he got to Hickory in 1944, there was an army tent pitched out front served as the admissions office. The buildings sat up on a hill, away from the road, and in the grass a patient sat on an ambulance stretcher. The hasty planning and architecture set Hickory apart from other hospitals, like Charlotte Memorial, that also housed polio patients.
At the hospital, treatments included “hot packs,” where boiled wool was placed on the skin, and extensive physical therapy. This contrasted with earlier treatments, which put serious patients in full body casts. When they got out, they often spent the rest of their lives unable to walk.
Thanks to his treatment at Hickory and a later series of operations, Moury has walked with a fairly normal gait his whole life.
Looking back, Dan remembers sleeping in a ward with about 15 or 20 boys about his age. They built model airplanes, played board games and, of course, went through physical therapy to get better.
“It was really a great year for me because I hated school — I was always in trouble,” he said. “And there wasn’t any school going on.”
***
To get the day's news and headlines in your inbox each morning, sign up for our email newsletters.
Researchers at UNC’s Southern Oral History Program are beginning a project to observe polio outbreaks, in light of the ongoing COVID-19 pandemic. Seth Kotch, the director of the program, said looking at polio is meant to provide “a different way of learning about what it’s like to live with a pandemic.”
The Hickory phenomenon is something researchers are interested in knowing more about, Kotch said. It involved a community rallying around medical professionals to fight a disease and treat children, most of whom weren’t even from Hickory. Kotch said echoes of that exist now, too, as health care workers come together to fight this pandemic.
But Kotch also sees echoes of the opposite: people mobilizing to spread misinformation about COVID-19 and the vaccine.
Dr. Myron Cohen, the director of UNC’s Institute for Global Health and Infectious Diseases, said people were far less hesitant to get the polio vaccine when it was developed and introduced in 1955.
“There were always people who were concerned about anything new,” Cohen said. “But there was certainly a lot more faith in science and scientists in the communications that existed in the ‘50s.”
Social media, the 24-hour news cycle, people seeking attention — these are all things Cohen suspects contribute to widespread hysteria about vaccines. Medical technology is remarkable, Cohen said, but the anthropological and sociological elements of society are suffering.
In other words, even the best vaccine isn’t effective if people refuse to get it.
When Moury took his son to get his polio vaccine at a school in Winston-Salem in the 1960s, he cried because he was so relieved his son would never have to go through what he did.
He likely wasn’t the only one. Parents everywhere lined up to get their children the long-awaited inoculation. More than 60 years since the first polio vaccine was developed, Cohen said the medical community still discusses polio vaccination programs as an example of global cooperation to wipe out a devastating disease.
To eradicate a disease, Cohen said, is “both amazing and romantic.”
“And to try and do it nowadays, with the way the world’s organized, would shockingly maybe be more difficult, not less difficult,” he said.
***
The local post-polio group now-85-year-old Moury belongs to used to have about 50 members. Just before COVID-19, it was down to four polio survivors who met for lunch once a month. Some died, while others moved away to be close to their children.
“We’re a dying breed,” he said.
As polio becomes medical history rather than a present threat, Moury has also noticed that fewer and fewer doctors know about Post-Polio Syndrome, a disorder that can show up in individuals who were once infected with polio.
And about 30 years ago, Moury went to an orthopedic surgeon for an elbow problem. Knowing that Moury had polio and had surgery as a child, the surgeon traced every incision on his foot and named the operation.
“We studied these, but I’ve never seen them before,” he told him.
Moments like these are reminders that polio is a thing of the past in the U.S. — and can remain that way if widespread vaccination continues. Researchers hope looking back at the moments in history when polio was widespread can help them shine a light on the pandemic the world faces right now.
“We want to learn about what it’s like for our country to live through, to endure, to suffer with a disease this serious,” Kotch said. “And what are the long-term effects of that experience?”
As for the hospital where Moury was treated so many decades ago, a historical marker stands in downtown Hickory to remind passersby of the miracle that occurred there. Moury, of course, was there the day they unveiled it.
Story and graphics originally produced for UNC Media Hub.
@MaeveSheehey
@DTHCityState | city@dailytarheel.com